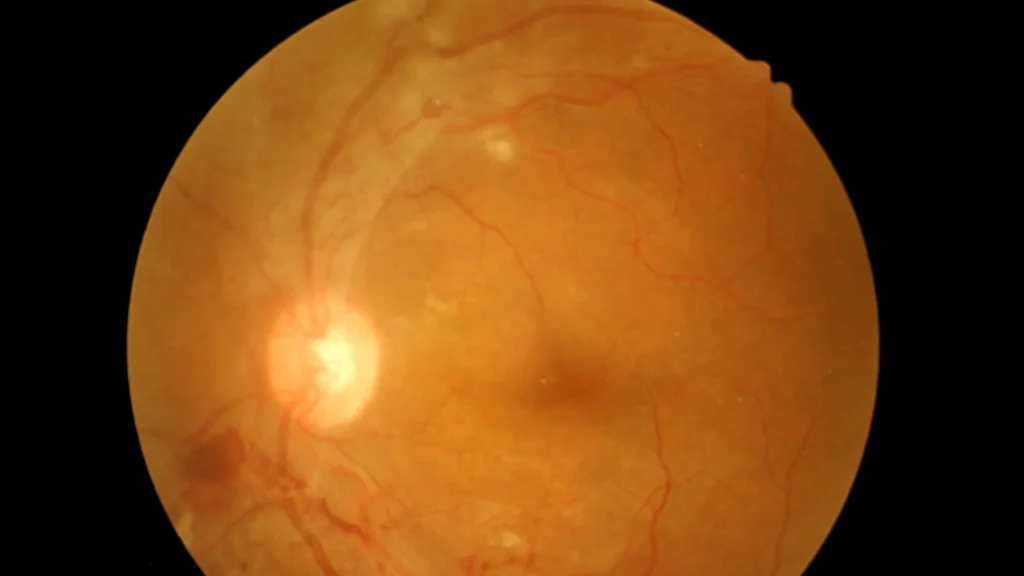
The gift of sight is precious, and maintaining the health of the delicate structures within the eye is paramount. At the back of the eye lies the retina, a light-sensitive layer responsible for sending visual information to the brain. Just like any other tissue, the retina requires a constant supply of oxygen-rich blood and an efficient drainage system. When the retinal veins, which carry deoxygenated blood away from the retina, become blocked, a serious condition known as retinal vein occlusion (RVO) occurs.
Retinal vein occlusion is one of the most common retinal vascular diseases after diabetic retinopathy, affecting hundreds of thousands of people each year. It is a critical condition that can lead to significant, sudden, and often permanent vision loss if not promptly diagnosed and managed by specialists. Understanding this disease—its causes, symptoms, and the advanced treatments available—is the first step toward preserving your sight. Here at Retina and Vitreous Surgeons of Utah (RSVU), we are committed to providing expert care for patients dealing with this complex diagnosis.
What Happens During a Retinal Vein Occlusion?
In a healthy eye, the central retinal artery brings blood to the retina, and the central retinal vein and its branches drain it. A retinal vein occlusion is essentially a “stroke” of the eye, where a blood clot or narrowing causes a blockage within one of these veins. This blockage prevents blood from leaving the retina, causing it to back up.
The resulting increase in pressure leads to hemorrhages (bleeding), swelling (edema), and a lack of oxygen (ischemia) in the affected areas of the retina. This damage to the retina’s sensory cells is what causes vision deterioration.
Specialists classify RVO into two main types, based on the location of the blockage:
- Central Retinal Vein Occlusion (CRVO): This is a blockage of the main central vein that drains the entire retina. Because the blockage is so extensive, CRVO typically causes more widespread and severe vision loss across the entire visual field.
- Branch Retinal Vein Occlusion (BRVO): This is a blockage in one of the smaller, tributary veins. BRVO is more common than CRVO, and while it may cause vision loss, the damage is often confined to the specific quadrant of the retina drained by that blocked branch, leading to a partial visual field defect.
Retinal Vein Occlusion: Root Causes and Risk Factors
RVO rarely occurs by chance; it is typically a complication of systemic health issues that affect the entire circulatory system. The most significant risk factors are often the same conditions that increase the risk of heart attack and stroke. These include:
- Systemic Hypertension (High Blood Pressure): This is the most prevalent risk factor. High blood pressure can cause the walls of the arteries to thicken and harden. Since a retinal artery and vein often share a common sheath at the artery-vein crossings, the hardened artery can press against and compress the softer vein, leading to a blockage.
- Diabetes: Poorly controlled blood sugar damages blood vessels throughout the body, including the retina, making them prone to blockages and leaks.
- Glaucoma: Elevated intraocular pressure (IOP) can place stress on the delicate structures where the central retinal vein exits the eye, increasing the risk of CRVO.
- Hyperlipidemia (High Cholesterol): High levels of circulating fats can contribute to clot formation.
- Age: The risk of developing retinal vein occlusion increases significantly with age, particularly after the age of 50.
- Blood Disorders: Certain rare conditions that cause the blood to clot more easily can also predispose an individual to RVO.
Symptoms and the Importance of Immediate Care
The hallmark symptom of a retinal vein occlusion is a sudden, painless blurring or loss of vision, usually in only one eye. The severity depends entirely on whether the blockage is a CRVO or a BRVO, and whether the central part of the retina (the macula) is involved.
Common symptoms include:
- Suddenly, noticeable blurring or a decrease in vision.
- Distortion of vision.
- Floaters (small spots or cobwebs that drift across the field of vision), caused by blood or fluid leakage.
- Pain is rare, making the condition particularly insidious.
If you experience any sudden change in your vision, it is crucial to seek immediate attention from a retina specialist. Early diagnosis of a retinal vein occlusion is vital for minimizing permanent damage.
The Path to Clearer Vision: Diagnosis and Treatment
Diagnosing RVO is typically straightforward and involves a comprehensive dilated eye examination. To confirm the diagnosis and assess the extent of the damage, our specialists utilize state-of-the-art imaging technology, including:
- Optical Coherence Tomography (OCT): This scan provides a detailed cross-section of the retina, allowing us to accurately measure the degree of macular edema (swelling), which is the primary cause of vision loss in RVO.
- Fluorescein Angiography (FA): A small amount of dye is injected into a vein in the arm, allowing the specialist to visualize the blood flow in the retinal vessels, pinpoint the location of the occlusion, and identify areas of poor circulation (ischemia) or abnormal blood vessel growth.
Treatment for retinal vein occlusion focuses primarily on reducing the macular edema and managing the growth of abnormal blood vessels (neovascularization), a serious complication that can lead to neovascular glaucoma and further vision loss. The gold standard treatments include:
- Intravitreal Anti-VEGF Injections: Medications that block Vascular Endothelial Growth Factor (VEGF), a protein that drives both swelling and abnormal blood vessel growth. These injections—such as Eylea (aflibercept), Lucentis (ranibizumab), or Avastin (bevacizumab)—are highly effective in reducing macular swelling and improving vision.
- Intravitreal Steroid Implants: Medications like Ozurdex (dexamethasone implant) or Iluvien (fluocinolone acetonide implant) are long-acting steroids injected into the eye to reduce inflammation and macular swelling.
- Laser Therapy (Photocoagulation): For areas of the retina with poor circulation (ischemia), a specialized laser can be used to prevent or treat abnormal blood vessel growth, typically in cases of BRVO or severe CRVO.
Partnering with RSVU for Optimal Outcomes
Managing a retinal vein occlusion is a long-term partnership between the patient and the retina specialist. Because RVO is tied to systemic health, managing underlying conditions like hypertension and diabetes is equally important for preventing recurrence in the affected eye and protecting the other eye.
If you or a loved one has been diagnosed with, or is experiencing symptoms consistent with, a retinal vein occlusion, specialized care is essential. The experienced team at Retina and Vitreous Surgeons of Utah (RSVU) uses the latest diagnostic tools and therapeutic protocols to stabilize the condition and restore as much vision as possible. Don’t delay—your sight depends on timely, expert intervention. To schedule a comprehensive evaluation or to learn more about our approach to treating retinal vein occlusion, please contact Retina and Vitreous Surgeons of Utah (RSVU).