The gift of sight is precious, and at Retina and Vitreous Surgeons of Utah, we are dedicated to helping you protect it. While many common eye conditions are manageable, some require immediate attention to prevent permanent vision loss. Among the most serious of these is retinal detachment, a medical emergency that can strike without warning. This guide covers retinal detachment symptoms and what to do if you suspect it. Our goal is to empower you with the knowledge to act decisively and protect your most valuable sense.
What is Retinal Detachment?
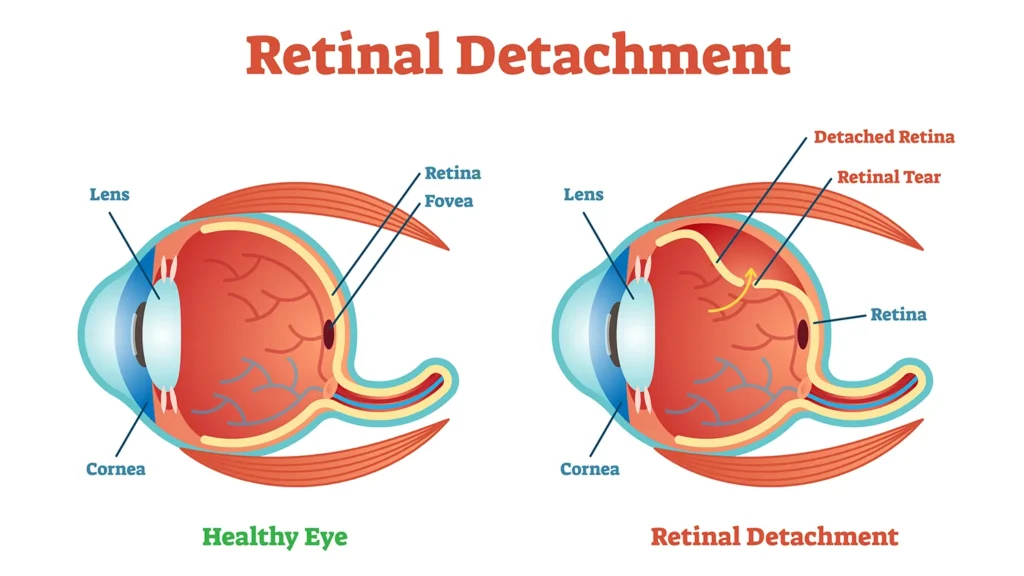
To understand retinal detachment, it helps to visualize the structure of the eye. The retina is a thin, delicate layer of tissue located at the very back of your eye. Its function is to receive light, convert it into neural signals, and send those signals to the brain, which then interprets them as images. Think of the retina as the film in an old-fashioned camera or the sensor in a digital one; without a properly functioning and correctly positioned retina, clear vision is simply not possible.
A retinal detachment occurs when this crucial layer of tissue pulls away from the layer of blood vessels that provide it with vital oxygen and nutrients. When the retina detaches, its cells are starved, and if the separation is not repaired quickly, it can lead to irreversible damage and permanent vision loss. There are three primary types of retinal detachment:
- Rhegmatogenous Detachment: This is the most common type, caused by a small tear or break in the retina. The tear allows fluid to seep underneath, causing the retina to peel away.
- Tractional Detachment: Often associated with conditions like advanced diabetes, this type happens when scar tissue on the retina’s surface contracts and pulls the retina away.
- Exudative Detachment: This occurs when fluid leaks from blood vessels into the space beneath the retina without any tears. It’s often linked to inflammatory diseases or tumors.
Regardless of the type, the result is the same: a separation that puts your vision in jeopardy.
The Warning Signs: Recognizing Retinal Detachment Symptoms
Prompt recognition of the warning signs is the most critical step in preserving your sight. The symptoms can be subtle at first and typically do not cause pain, but they demand immediate action. If you experience any of the following retinal detachment symptoms, it’s a call to action, not a cause for delay:
- A Sudden Increase in Floaters: While many people experience harmless floaters—specks or “cobwebs” that drift across their vision—a sudden, dramatic increase in their number is a major red flag. This can be described as a “shower” of new specks that weren’t there before.
- Flashes of Light (Photopsia): These are brief, sparkling flashes of light that often appear in the peripheral (side) vision. They can be more noticeable in a dark room. These flashes are caused by the retina being pulled or tugged.
- A Dark “Curtain” or Shadow in Your Field of Vision: This is often the most definitive and alarming symptom. It may start small and grow over time, but it appears as a dark, gray, or black shadow or a curtain-like shape that moves from the edge of your vision inward. This signifies that a portion of the retina has already detached.
- Blurred or Decreased Vision: As the detachment progresses, it can affect the central part of the retina, known as the macula. When this happens, you may notice your vision becoming distorted, blurry, or significantly diminished.
It is crucial not to dismiss these symptoms. While they can sometimes be caused by other conditions, the risk of permanent vision loss from retinal detachment is too high to ignore.
What to Do If You See Retinal Detachment Symptoms: The Critical Next Steps
If you experience any retinal detachment symptoms, you are in a time-sensitive medical emergency. Every minute counts. Here is what you need to do immediately:
- Do Not Wait. Do not try to “wait and see” if the symptoms go away. Do not wait for a regularly scheduled appointment. The clock is ticking.
- Contact a Retina Specialist Immediately. The best course of action is to call an ophthalmologist who specializes in retina care directly. At Utah Retina, we have a team of specialists who are equipped to handle these emergencies. Explain your symptoms clearly and tell them you suspect retinal detachment.
- Go to an Emergency Room. If you cannot reach a retina specialist right away, go to the nearest emergency room. They can provide initial care and, most importantly, connect you with an on-call ophthalmologist.
Retinal Detachment: The Path to Recovery
The good news is that with prompt diagnosis and modern surgical techniques, retinal detachment is a highly treatable condition. The goal of all treatments is to reattach the retina to the back wall of the eye and seal any tears. Depending on the severity and location of the detachment, our specialists may recommend:
- Laser Surgery (Photocoagulation): Used for small tears before a full detachment, a laser creates tiny burns that weld the retina to the underlying tissue.
- Pneumatic Retinopexy: A gas bubble is injected into the eye to push the retina back into place, and a freezing probe or laser is then used to seal the tear.
- Vitrectomy: This microsurgery involves removing the vitreous gel from the eye, reattaching the retina, and then injecting a gas or silicone oil bubble to hold it in place while it heals.
Your vision is one of your most valuable assets. By being informed about retinal detachment symptoms and knowing how to respond, you can be your own best advocate in a moment of crisis. Regular comprehensive eye exams are the best way to monitor your eye health and catch any issues early. If you have any concerns about your vision or are at high risk for retinal detachment, please contact us at RVSU. Your sight is our priority.